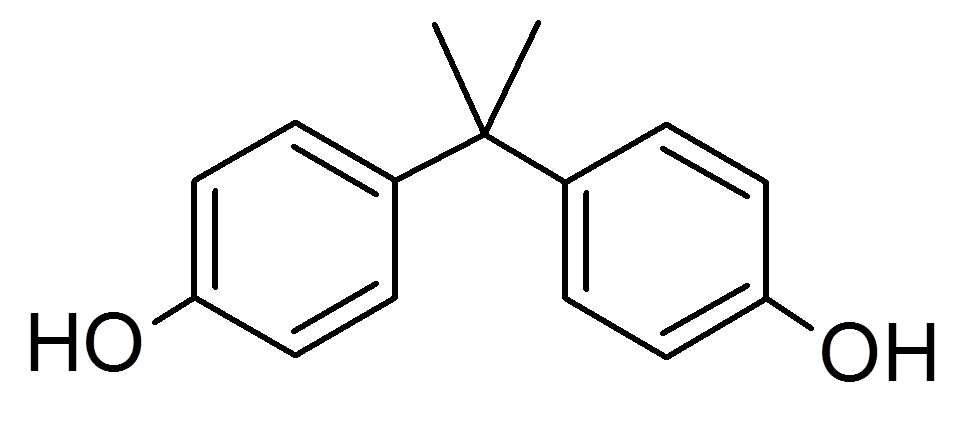
1. Chemistry, applications and regulation
Bisphenol A (BPA, CAS 80-05-7) is mainly used as a starting substance for polycarbonate plastics and epoxy resins. Polycarbonates (PC) plastics applications include glasses, electronics and solar panels. In food contact materials, PC plastic is used to manufacture refillable water containers for water dispensers and other PC electronic kitchen appliances. Epoxy resins are used as coatings in lids of glass containers and in the linings of aluminum cans. Further BPA is used to coat thermal papers. EFSA’s latest draft scientific opinion (part I) highlights that diet is the major contributor to BPA exposure [1].
Global production capacities of BPA have exceeded 2 million tons since the turn of the 21stcentury. BPA was first synthesized in 1891 and first found to exhibit estrogenic activity in the 1930s [2, 3]. The Reference Dose for Chronic Oral Exposure (RfD) was set to be 0.05 mg/kg body weight/day by the US EPA, based on the lowest observed effect level of 50 mg/kg body weight/day [4]. Also in the European Union the TDI is set at 0.05 mg/kg body weight/day and a Specific Migration Limit (SML) of 0.6 mg/kg food has been regulated in 2012 [5, 6]. In January 2014 the European Food Safety Authority (EFSA) published a draft scientific opinion (part II) on the assessment of risks to human health of BPA and recommended that the TDI should be lowered to 5 µg/kg body weight/day [7]. Awaiting the findings of research carried out by the U.S. National Toxicology Program (NTP), which are to be expected in 2015, the newly proposed TDI should be set on a temporary basis.
2. Toxicity
Since the beginning of the 90s BPA has been the subject of increased scientific investigation regarding its estrogenicity. Scientists have found BPA to interact with estrogen receptors, both in the nucleus as well as on the cell membrane, to be an androgen receptor antagonist and to reduce the synthesis of some steroids at the molecular level [8-10]. In vitro studies have found low-dose effects of BPA on adipose, reproductive and mammary tissue, the immune and nervous system, the liver and in pancreatic and pituitary models [11]. In in vivo models exposure levels below 50 mg/kg body weight/day have been observed to cause changes in brain physiology, brain structure, behavior, and sex differences in the brain. In females, fertility and the onset of puberty were affected by BPA. Furthermore, BPA caused changes in the mammary gland, uterus, vagina, ovary oocytes and affected the immune system and metabolism of test animals [12]. Further, effects such as carcinogenesis and adipogenesis, as well as changes in male reproduction have been recently added to the list [13, 14].
In epidemiological studies associations of BPA exposure and diabetes, cardiovascular disease and altered liver enzyme levels were found. Further, decreased semen quality, sperm DNA damage, altered thyroid function, metabolic syndrome, obesity, hypertension, peripheral arterial disease and coronary arterial stenosis could be associated with BPA exposure [15-26].
Yet consensus regarding the health risks of BPA has not been established in the scientific community and discussion on the risk evaluation of BPA has been ongoing since the 1990s. Particular points of debate include whether all rodent strains used as test animals are equally sensitive to hormonally active compounds and whether positive controls should be included in Good Laboratory Practice (GLP) studies. Further, the neglect of results as well as the lack of certain endocrine relevant endpoints in GLP studies have been criticized. There also exists a continuous debate about windows with increased sensitivity to exposure and the accuracy of extrapolation from the animal model to humans. The last point of debate is the quantification of biologically active BPA (“free” or unconjugated BPA) in human blood samples, as some studies have found BPA conjugation (inactivation) to be less permanent than previously thought [27]. Another source of uncertainty is the inadvertent contamination of biomonitoring samples by the ubiquitous presence of BPA traces in laboratories [28].
Two multigenerational reproduction studies were carried out in accordance with GLP and unable to confirm the findings of academic research [29, 30]. They have provided the basis of regulatory risk assessment. Yet, public concern has resulted in a ban of BPA from packaging and reusable food containers intended for children under the age of 3 in Canada, the European Union and the United States. On the basis of a reevaluation carried out by the French National Agency for Food, Environmental and Occupational Health & Safety (ANSES), the French National Assembly and Senate voted in the end of 2012 to ban BPA from all food contact products by January 2015 (Proposition N°49). The CLARITY-BPA study was carried out within the US to address disagreement surrounding the use of traditional endpoints of toxicity and modern hypothesis-driven, disease-relevant outcomes in previously studied animals. A study was published in 2021 that evaluates 20 years’ worth of BPA studies, including results from the CLARITY-BPA study [31].
3. References
1. CEF. 2013. Draft scientific opinion on the risks to public health related to the presence of bisphenol A (BPA) in foodstuffs – Part: exposure assessment. EFSA Journal.
2. Dodds EC, and Lawson W. 1938. Molecular structure in relation to oestrogenic activity. Compounds without a phenanthrene nucleus. Proc R Soc Lond B. 125:222-32.
3. Dodds EC, and Lawson W. 1936. Synthetic oestrogenic agents without the phenanthrene nucleus. Nature. June 13:996.
4. US EPA. 2002. Integrated Risk Information System: Bisphenol A.
5. CEF. 2010. Scientific opinion on bisphenol A: evaluation of a study investigating its neurodevelopmental toxicity, review of recent scientific literature on its toxicity and advice on the Danish risk assessment of bisphenol A. The EFSA Journal. 8:1829.
6. European Commission. 2002. Commission Directive 2002/72/EC of 6 August 2002 relating to plastic materials and articles intending to come into contact with foodstuffs. Official Journal of the European Communities.
7. CEF. 2014. Draft scientific opinion on the risks to public health related to the presence of bisphenol A (BPA) in foodstuffs. EFSA Journal.
8. Wolstenholme JT, Rissman EF, and Connelly JJ. 2011. The role of Bisphenol A in shaping the brain, epigenome and behavior. Horm Behav. 59:296-305.
9. Kuiper GGJM, Lemmen JG, Carlsson B, et al. 1998. Interaction of estrogenic chemicals and phytoestrogens with estrogen receptor beta. Endocrinology. 139:4252-63.
10. Dolinoy DC, Huang D, and Jirtle RL. 2007. Maternal nutrient supplementation counteracts bisphenol A-induced DNA hypomethylation in early development. P Natl Acad Sci USA. 104:13056-61.
11. Wetherill YB, Akingbemi BT, Kanno J, et al. 2007. In vitro molecular mechanisms of bisphenol A action. Reprod Toxicol. 24:178-98.
12. Richter CA, Birnbaum LS, Farabollini F, et al. 2007. In vivo effects of bisphenol A in laboratory rodent studies. Reprod Toxicol. 24:199-224.
13. Gies A, and Soto AM. 2012. Bisphenol A: contested science, divergent safety evaluations, Lessons from health hazards. European Environment Agency. pp 247-71.
14. Allard P, and Colaiacovo MP. 2011. Bisphenol A. In: Reproductive and Developmental Toxicology. R.C. Gupta, ed. Elsevier, München. pp 673-86.
15. Lang IA, Galloway TS, Scarlett A, et al. 2008. Association of urinary bisphenol A concentration with medical disorders and laboratory abnormalities in adults. JAMA. 300:1303-10.
16. Melzer D, Rice NE, Lewis C, et al. 2010. Association of urinary bisphenol A concentration with heart disease: evidence from NHANES 2003/06. PLoS One. 5:e8673.
17. Sugiura-Ogasawara M, Ozaki Y, Sonta S, et al. 2005. Exposure to bisphenol A is associated with recurrent miscarriage. Hum Reprod. 20:2325-9.
18. Mok-Lin E, Ehrlich S, Williams PL, et al. 2010. Urinary bisphenol A concentrations and ovarian response among women undergoing IVF. Int J Androl. 33:385-93.
19. Cantonwine D, Meeker JD, Hu H, et al. 2010. Bisphenol a exposure in Mexico City and risk of prematurity: a pilot nested case control study. Environ Health. 9:1-7.
20. Li DK, Zhou Z, Miao M, et al. 2011. Urine bisphenol-A (BPA) level in relation to semen quality. Fertil Steril. 95:625-30.
21. Meeker JD, Ehrlich S, Toth TL, et al. 2010. Semen quality and sperm DNA damage in relation to urinary bisphenol A among men from an infertility clinic. Reprod Toxicol. 30:532-9.
22. Braun JM, Yolton K, Dietrich KN, et al. 2009. Prenatal bisphenol A exposure and early childhood behavior. Environ Health Perspect. 117:1945-52.
23. Shankar A, and Teppala S. 2012. Urinary bisphenol A and hypertension in a multiethnic sample of US adults. J Environ Public Health. 2012:481641, 5 pages.
24. Shankar A, Teppala S, and Sabanayagam C. 2012. Urinary bisphenol A levels and measures of obesity: results from the national health and nutrition examination survey 2003-2008. ISRN Endocrinol. 2012:1-6.
25. Shankar A, Teppala S, and Sabanayagam C. 2012. Bisphenol A and peripheral arterial disease: Results from the NHANES. Environ Health Perspect. 120:1297-300.
26. Teppala S, Madhavan S, and Shankar A. 2012. Bisphenol A and metabolic syndrome: Results from NHANES. Int J Endocrinol. 2012:598180.
27. Patterson TA, Twaddle NC, Roegge CS, et al. 2013. Concurrent determination of bisphenol A pharmacokinetics in maternal and fetal rhesus monkeys. Toxicol Appl Pharmacol. 267:41-8.
28. Ye X, Zhou X, Hennings R, et al. 2013. Potential external contamination with bisphenol A and other ubiquitous organic environmental chemicals during biomonitoring analysis: an elusive laboratory challenge. Environ Health Perspect. 121:283-6.
29. Tyl RW, Myers CB, Marr MC, et al. 2008. Two-generation reproductive toxicity study of dietary bisphenol a in CD-1 (Swiss) mice. Toxicol Sci. 104:362-84.
30. Tyl RW, Myers CB, Marr MC, et al. 2002. Three-generation reproductive toxicity study of dietary bisphenol A in CD Sprague-Dawley rats. Toxicol Sci. 68:121-46.
31. vom Saal FS, Vandenberg LN, Marr MC, et al. 2021. Update on the Health Effects of Bisphenol A: Overwhelming Evidence of Harm. Endocrinology 162:3.